Healthcare changemakers
Uncovering new insights to power transformation
Richard Clarke, Chief Analytics Officer of Highmark Health, builds trust and drives transformation by surfacing new insights for providers.
Specialty care costs are growing 4.5x faster than primary care. Health plans need a different approach to lower risk and manage costs.
Clarify Health is an elite Provider analytics platform supported by a great IT team. They were able to ingest our very large dataset without any issues… The tool itself is easy to use and offers practitioner insights that are a notch above other vendors.”
Analytics precision to unlock savings
Achieve savings and improve outcomes by identifying the best providers, targeting specific changes, and directly engaging physicians on care.
Own the best networks
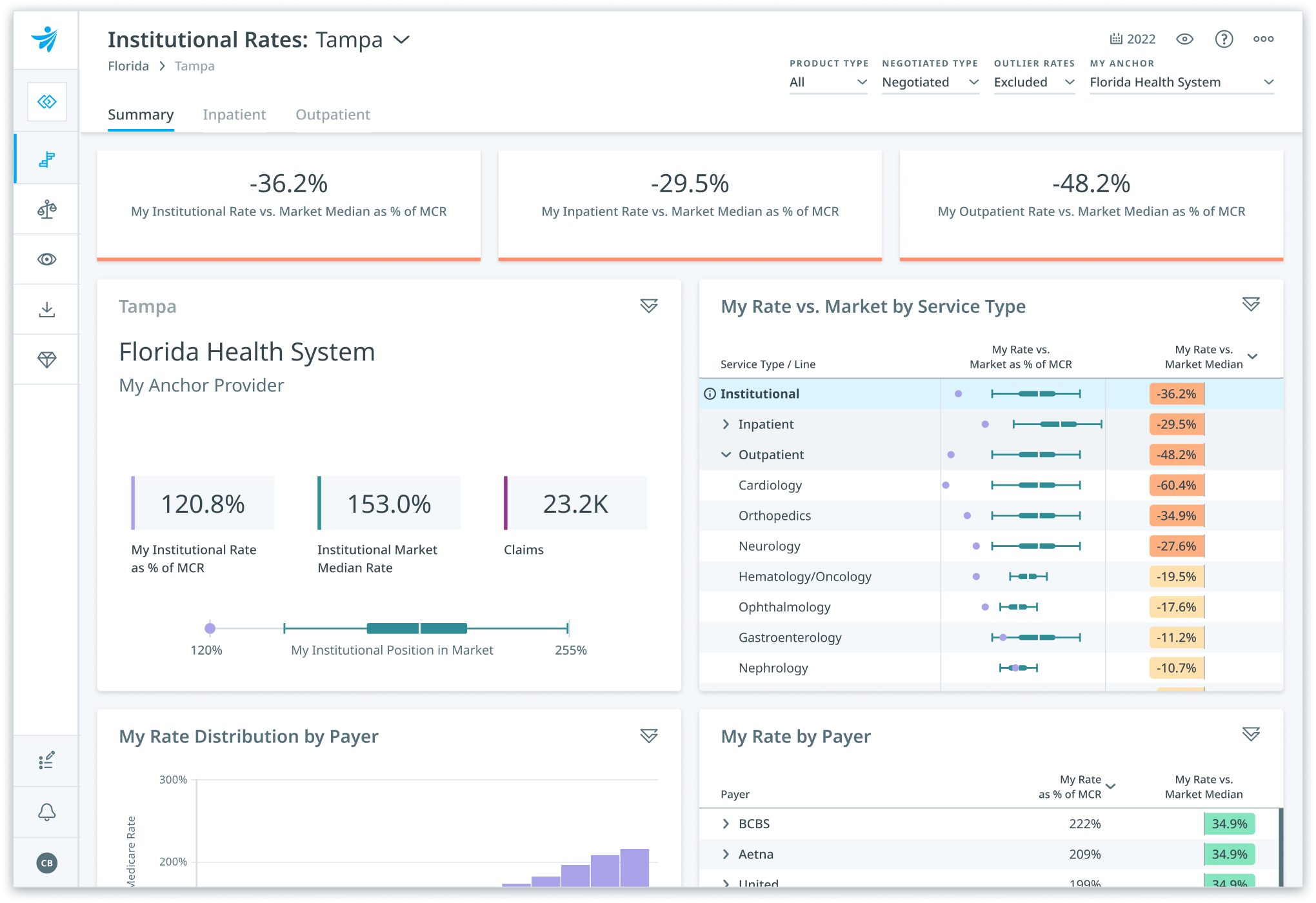
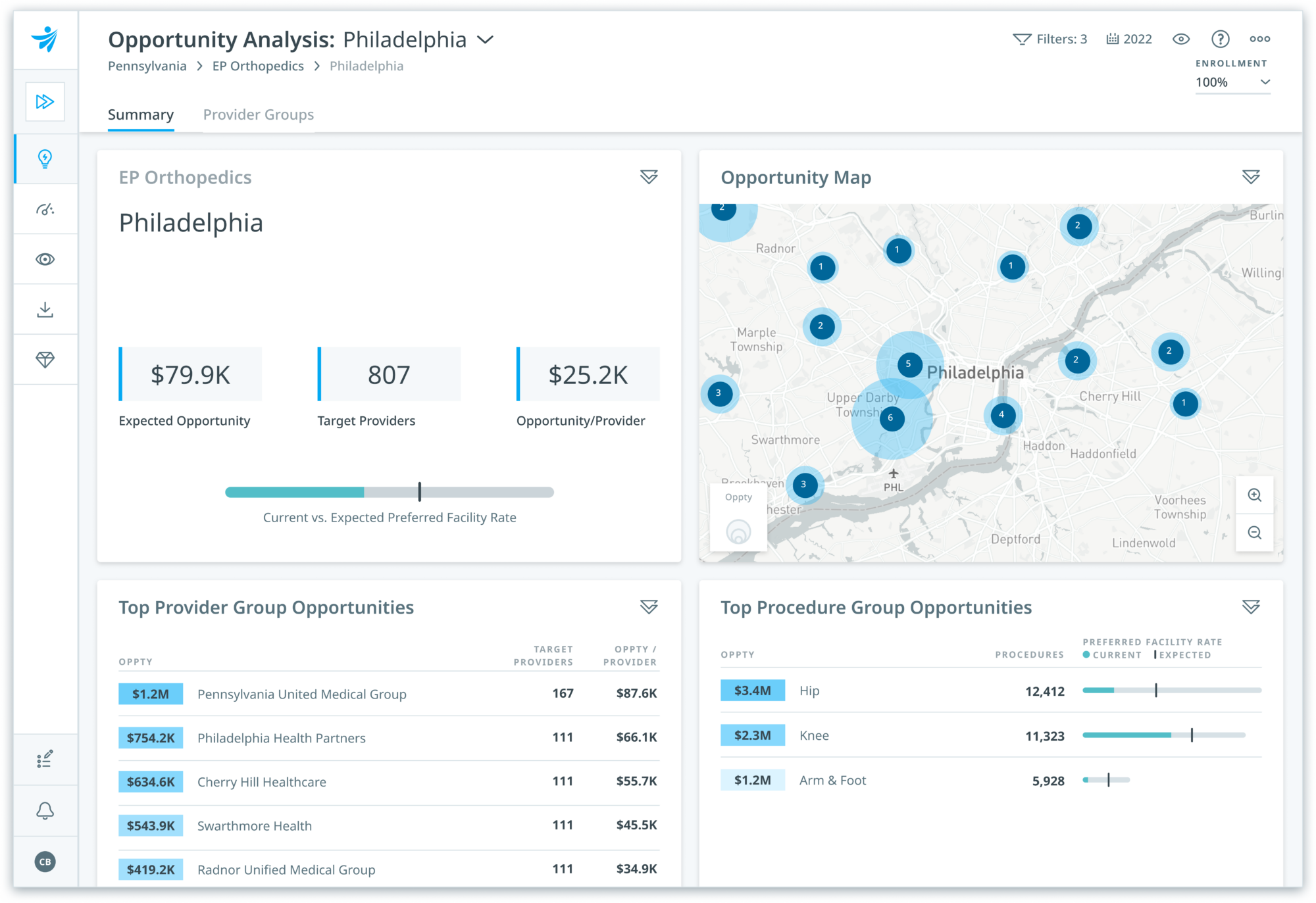
Pinpoint the right opportunities
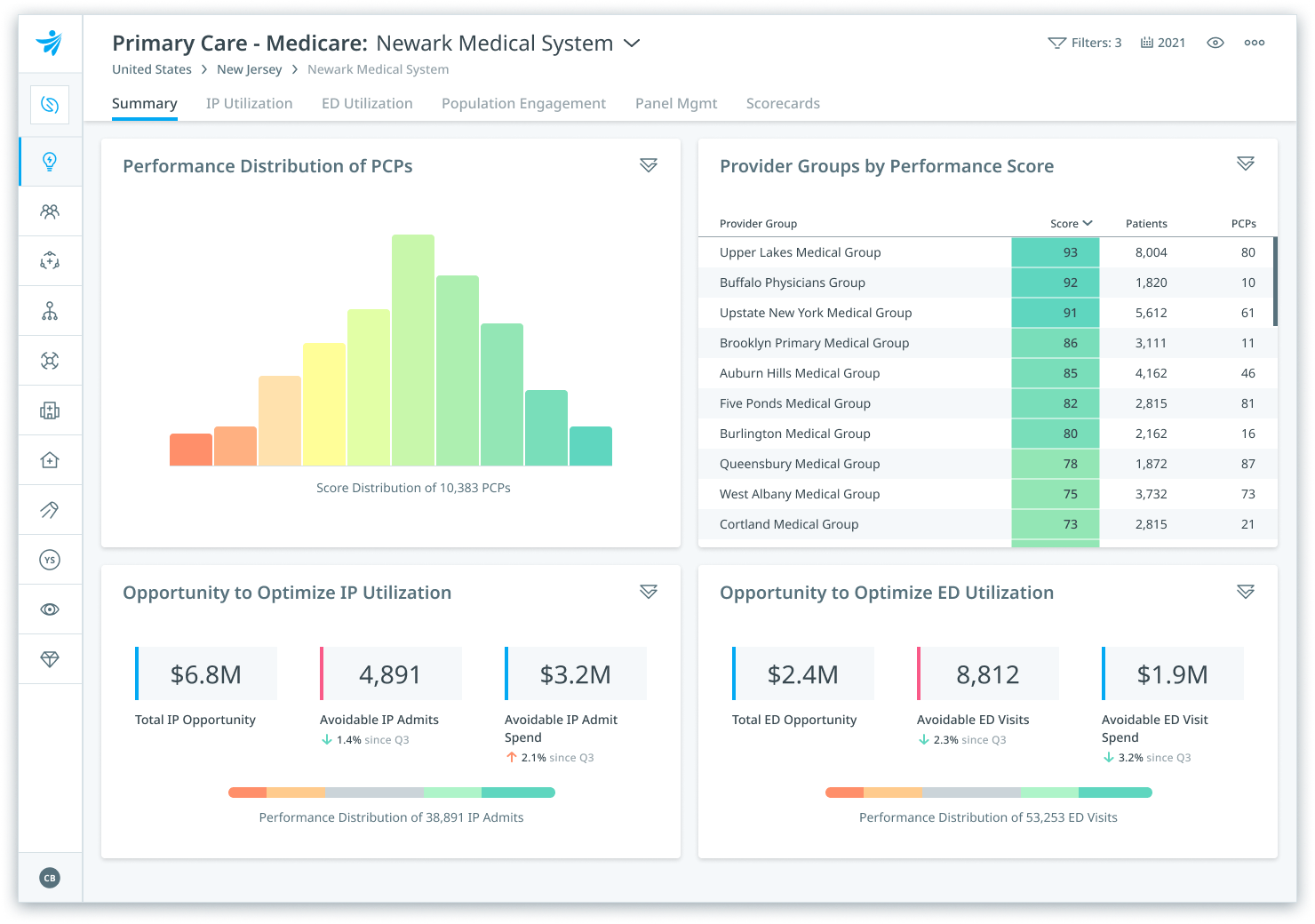
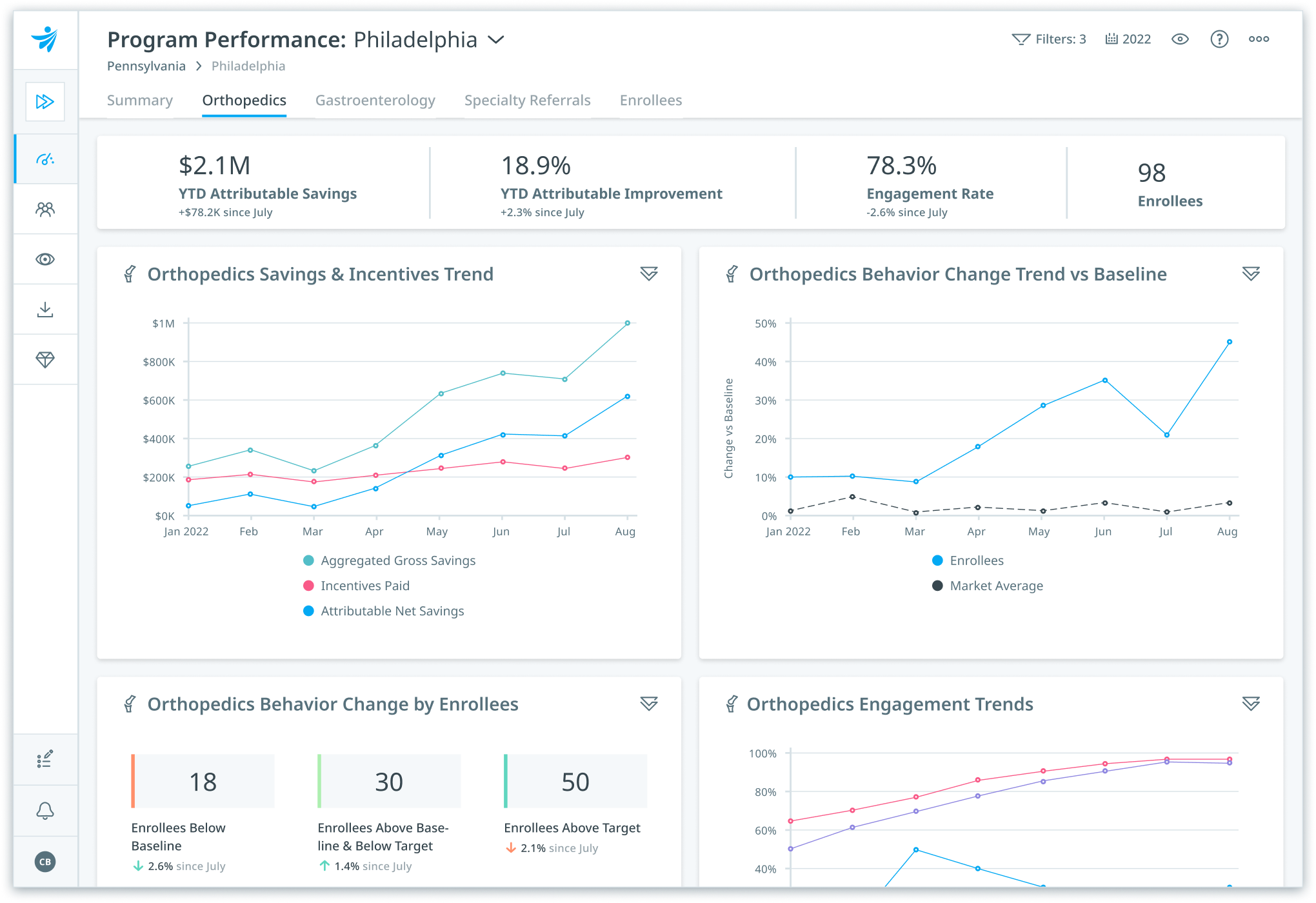
Reduce medical spend

$285M
in clinical cost savings identified
$500M
in net new MA revenue in 1 year
6:1
$6 in savings generated for every $1 incentive spent
$70M
year-1 VBC contracting savings
What I like most about Clarify Health are the data and the customer support. Clarify provides a user-friendly platform that provides data analytics at the tip of our fingers.”
Clarify is a great partner for fast, high-quality insights.”
Clarify is showing us which providers/health systems are in-network with our top competitors where we’re doing business. It gives us a roadmap to mirroring our competitors’ 4-5 Star plans. It also adds value by giving a view into volume (attributed patients) and performance (quality/efficiency scores) as we tailor provider targets.”
Insights for Payers
Insights for Payers
Insights for Payers
Insights for Payers
Insights for Payers
Insights for Payers
Insights for Payers
Insights for Payers
Insights for Payers
Insights for Payers
Insights for Payers
Insights for Payers
Insights for Payers
Insights for Payers
Insights for Payers
Insights for Payers
Insights for Payers
Insights for Payers
Insights for Payers
Insights for Payers
Insights for Payers
Insights for Payers
Insights for Payers
Insights for Payers
Insights for Payers
Insights for Payers
Insights for Payers
Insights for Payers
Insights for Payers
Insights for Payers
Insights for Payers
Insights for Payers
Insights for Payers
Accelerate transformation, drive growth, and adopt innovative payment models confidently with the industry’s most trusted healthcare analytics platform, mapping over 300 million real-world patient journeys with machine-learning precision.